After a 10-year long battle as a Type 2 Diabetic, I was diagnosed as insulin-dependent Type 2 Diabetic (T2D) at the age of 46. This sudden change in my health has had me feeling lost and confused more times than not. What is a carbohydrate? When should I take insulin? How can I help my Type 2 body better use the insulin it produces? How different is life for a Type 2 diabetic on insulin than a Type 1 diabetic (T1D)? What resources are available to help me learn to treat this new disease? In this article, I will explore life as a T2 diabetic on insulin and what I have learnt during this journey.
AS A QUALIFIER: The following should be considered as personal experience and observations. However, I am not a medical professional and any information or questions you have should be discussed with your healthcare team. With that in mind, I hope this will be of some use to you. I would also like to extend my thanks to Lilly Canada for sponsoring this education article.
Table of Contents
- What is the difference between Type 1 Diabetes, Type 2 Diabetes and Gestational diabetes?
- The Typical Progression of Type 2 Diabetes
- Type 2 Diabetes: The older we get, the more complicated the treatment
- My Type 2 Diabetic Diagnosis and Seniors
- Lessons I have had the Learn the Hard Way as a Type 2 Diabetic on Insulin
- Insulin Dosing Mistakes as a Type 2 Diabetic and Hypoglycemia Scares
- Hypoglycemic Education
- Learning the Diabetes Ropes from T1D Community
According to research lead by the Public Health Agency of Canada, in 2013–2014, close to 200,000 Canadians were newly diagnosed with diabetes (5.9 per 1,000 population). This represented 0.4 new cases per 1,000 population among children and youth and 7.6 new cases per 1,000 population among adults. At least I know I am in good company. When I was diagnosed in 2008, I was one of the 4 per 1000 of the lucky Canadian population in my age group that shared the disease.
What is the difference between Type 1 Diabetes, Type 2 Diabetes and Gestational diabetes?
The government of Canada’s Chronic Disease Surveillance System (i) defines diabetes as a chronic condition that occurs when the body loses its ability to produce or properly use insulin, a hormone that controls sugar levels in the blood. There are three main types of diabetes: type 1, type 2 and gestational diabetes. Other types are uncommon.
What is Type 1 diabetes (T1D)?
Type 1 diabetes is an autoimmune disease. The immune system destroys the insulin-producing cells of the pancreas, leaving the individual dependent on an external source of insulin for life. Type 1 diabetes typically develops in children and youth, but it can also occur in adults.
What is Type 2 diabetes (T2D)?
Type 2 diabetes is a metabolic disorder. Type 2 diabetes occurs when the pancreas does not produce enough insulin and/or when the body does not properly use the insulin produced. Individuals who are overweight or obese, physically inactive, or of certain ethnic origins, and those who have a family history of diabetes are more likely to develop type 2 diabetes. T2 typically appears in adults older than 40 years, but it can also occur at a younger age, for me I was in my mid-thirties.
What is Gestational diabetes?
Gestational diabetes occurs in pregnant women if high blood sugar levels develop during pregnancy. Although it usually disappears after the delivery, it increases the risk of developing type 2 diabetes later.
It has been estimated that 90% of diabetes cases among Canadian adults are Type 2, 9% Type 1, and less than 1% of a different type, while the large majority of diabetes cases among children and youth are Type 1. Moreover, gestational diabetes is reported in about 5.5% of births.
The Typical Progression of Type 2 Diabetes
Unlike Type 1, whose bodies suddenly begin destroying insulin-producing cells, Type 2 diabetes, like me, is a progressive disease that can lead to a lifestyle that echo’s Type 1 diabetes and the risks and dangers associated to hypoglycemia and hyperglycemia in addition to the progressive long term risks of diabetes including Eye damage, heart disease and stroke, high blood pressure, kidney disease, mental health issues, and nerve damage and amputation
Dr Vivian A. Fonseca (2), describes the progression of Type 2 diabetes as 5 stages. Dr Fonseca notes that the path to pre-diabetes can begin as early as 12 years before diagnosis, with the progression in a decline in β–cell function, and continues throughout the disease process. The primary function of the β–cell or Beta Cell is to produce and release insulin and amylin. Both are hormones which reduce blood glucose levels.
Stages of Progression of Type 2 Diabetes
- Stage 1: Pre-Diabetes Diagnosis
- Stage 2: Progression from pre-diabetes to overt diabetes.
- Stage 3: Acute insulin response
- Stage 4: Progression to medication
- Stage 5: Loss of glycemic control on medication – Insulin Dependence
The speed and rate of progression are dependent on many influences, however, include High BMI (body mass index), Weight gain, age of progression, High plasma insulin, Decreased insulin response to glucose, Dyslipidemia, Hypertension, Poor β-cell function and choice of treatment.
Type 2 Diabetes: The older we get, the more complicated the treatment.
What is clear is that Type 2 diabetes is a progressive disease whose treatment requirements increase in complexity, from management with diet and exercise, to medication, and eventually to insulin dependence. This is even more important when you consider there is typically a positive correlation between age and the progression of Type 2 Diabetes. The older we get, the more complicated the treatment.

While less than 1 in 1000 Canadians under the age of 30 are diagnosed with diabetes each year. This increases to over 10 in a 1000 Canadians by age 55 and over 20 in a 1000 Canadian men, and nearly 15 in a 1000 Canadian women over the age of 70 are diagnosed with diabetes each year. What age-appropriate resources are available to Type 2 diabetics? Where can we learn about how to change our habits and lifestyle to slow the progression of the disease, diet tips, eating tips? Truth be told, I don’t think I could even tell you what a carbohydrate was when I was first diagnosed.
Here are some of the great diabetes education resources I have used over the years:
Local Diabetes Clinic
Without a doubt, the endocrinologists, diabetes nurses, dietitians, and kinesiologists at my local diabetes clinic rock. Don’t get me wrong, my endocrinologist gives me a 5-minute lesson on counting carbs and insulin dosing, however, my diabetes nurse is where the real education begins. I highly recommend any diabetic ask for a referral to their local diabetes clinic.
When I was first diagnosed as a Type 2 diabetic the diabetes clinic had a half-day class on what it means to be a diabetic. I admit, at 36 I was by far the youngest in the class. However, I walked away with valuable lessons on portion control, low-glycemic foods, and that exercise doesn’t need to be the gym. They also offered separate classes on bodyweight exercises, cooking and shopping classes and more.
Speak to your family physician, endocrinologist, or nurse practitioner for a referral. You can also check with the clinic to see if they have a self-referral process.
Diabetes Instagram and Facebook Groups
One of the reasons I write in my blog is to extend the knowledge and experience I have gained as a diabetic. Everyone takes away different experiences when it comes to life, and in my case dealing with diabetes and Crohn’s disease. If nothing else, it is great to know we are not alone. Although, we can usually walk away with so much more. User groups and forums, and more recently Facebook Groups on Diabetes (Diabetes Canada and Type 2 Diet and Support Canada – Type 2 Diabetes) can be great resources to get firsthand information.
Surprisingly enough – Instagram has been another great resource for both motivation but as well as knowledge. Much like the posts on my IG Account, many members of the diabetes community post about their lessons, successes, and failures. It is great to know we are not alone. A special shout out to Jessie Inchauspe (GlucoseGoddess), although she isn’t a diabetic her playful use of Continuous Glucose Monitors (CGM) like the Freestyle Libre, give us a great visual reminder of how a normal person body responds to a balanced diet. How close can I get my diabetic body?
Diabetes Websites and Recommended Books
Much like you are doing now, self-help is the last of my resources, although maybe one of the most important. Self-help equates entirely to ownership, which is the first tool in transitioning our lifestyles to be diabetic friendly. Don’t get me wrong, I have my cheat days – that’s what keeps me sane. After all, two chronic diseases can be a bit of an emotional roller coaster at times.
Some of my favourite sources are as follows:
- https://www.diabetesselfmanagement.com/ – basic information on diabetes and lots of recipes
- https://asweetlife.org/ – updates on products and technologies, recipes, and more
- https://www.type1writes.com/ – Frank writes about his T1 journey
- https://diatribe.org/ – online publication, covers basic diabetes information, products, tech, drugs, and more.
- Exercise Videos – http://guidelines.diabetes.ca/patient-videos – Step by step videos on resistance band and dumbbell workouts. Be sure to check with your physician before starting any workout routine.
Type 2 Diabetic Diagnosis and Seniors
As I touched on earlier – I started my diabetes journey in my mid-thirties. I am educated, research and internet savvy, although stubborn, not completely set in my ways, I exercise, although eat out a bit too often. However, all in all, I had my whitts to be able to help understand what it meant to my lifestyle to be diagnosed as a diabetic.
Don’t get me wrong – I hated the diagnosis and constantly tested my life and body without the dependence on medicine to manage my blood sugars. The reality is, I am a diabetic and in my case, an insulin-dependent Type 2 diabetic. As my readers also know, I also have Crohn’s disease.
Much like a Type 1 Diabetic (T1D), I need to test my glucose before each meal to determine how much bolus (fast-acting) insulin I need to take to balance my carbohydrates, and basal insulin at bedtime. As a Type 2 diabetic, I also benefit from oral medications that boost my body’s ability to naturally manage my glucose. Even after over 10 years of being a diabetic progressing through the stages of Type 2, I am still learning and more importantly still making mistakes, some of which can have serious and life-threatening consequences like hypoglycemia.
In my defence, it has been a moving target on how to manage my diabetes as I progressed from a Stage 2 Type 2 Diabetic to a to Stage 5 T2 Diabetic (see the stages above). My newest struggle, what does it mean to be insulin-dependent? This also has me wondering, If I am struggling as an adult learning how to manage daily life needing to take insulin, how well would senior citizens manage the same progression of their Type 2 Diabetes? What is even of bigger concern – how well would a senior citizen with progressive cognitive impairments such as Alzheimer’s disease (AD) or Dementia cope with managing sever Type 2 diabetes, or even more importantly their caregivers?
What resources are available, to learn, educate, and survive our diabetes journies that is age-appropriate? If I can use my parents as examples, I certainly learn much differently than they do in their 70’s.
Lessons I have had the Learn the Hard Way as a Type 2 Diabetic on Insulin
If you read any forum or newsgroup about Type 2 Diabetes, two of the biggest concerns expressed are:
“I don’t like needles, I never want to be on Insulin”, or
“I am very afraid of my sugars going too low”, a situation otherwise known as hypoglycemia. In fact, research shows that 60% of Type 2 Diabetics modify their insulin doses after a hypoglycemic event. Not a good statistic!
Insulin Dosing Mistakes by a Type 2 Diabetic and Hypoglycemia Scares
I have made tones of mistakes in my short time living with insulin. How much insulin should I take, when should I take it, should I take insulin if I have a snack. I was literally given a prescription for Humalog (Fast-Acting Insulin), a sliding scale based on what my pre-meal glucose was, and fingers crossed, sent on my way.
I admit it was overwhelming, scary, and naturally, a bit of a pain to suddenly be dependent on carrying around diabetic supplies: insulin, needles, my glucometer or CGM, and snacks for low sugar events such as Dex4 glucose tablets. I made mistakes! As much as I have amazing things to say about my diabetes clinic, when it comes to suddenly being thrown into the lifestyle of a T1 Diabetic – I feel that insulin-dependent Type 2 Diabetics seem to bet missed in the shuffle, with resources for parents of recently diagnosed T1D children, and traditional diet and medication dependent T2D. However, as recently diagnosed T1D adults (or equivalents) – we seem to need to depend on asking our own questions and answers and do not have the right appreciation of the risks.
Severe Hypoglycemia Experiences
What is Hypoglycemia?
Hypoglycemia, also known as low blood sugar, is a condition caused by a very low level of blood sugar (glucose), your body’s main energy source.
Immediate treatment of hypoglycemia is necessary when blood sugar levels are at 70 milligrams per deciliter (mg/dL) or 3.9 millimoles per litre (mmol/L) or below. Treatment involves quick steps to get your blood sugar level back into a normal range either with high-sugar foods or drinks or with medications. Long-term treatment requires identifying and treating the underlying cause of hypoglycemia.

For Canadians who have diabetes and who are treated with insulin, the fear of going ‘low’ (hypoglycemia) never goes away. When an individual has a severe low (severe hypoglycemia), they are unable to treat themselves, and they need help. For people with Type 1 or Type 2 diabetes who are on medications like insulin, there can be countless causes of severe hypoglycemia. These include not eating enough, over-exercising, drinking alcohol, or even using diabetes medications incorrectly.iii
There are different levels of low blood sugar: mild, moderate, or severe. If your blood sugar drops low enough that you need help to recover, it is considered to be a low blood sugar emergency or severe hypoglycemia.
My Pre-Bolus (Fact Acting Insulin) Oops
It is recommended that diabetics pre-bolus our fast-acting insulin 10-30 minutes before eating in order to most accurately mimic the insulin response of a non-diabetic. This will help assist in your blood sugars not spiking before out insulin starts to work.
What I ended up learning by mistake – pre-bolusing requires a guaranteed eating time and carbohydrate amounts. This past summer (about 6 months into being insulin-dependent) my pre-bolusing at a restaurant created a very scary and escalating problem when our food was delayed due to a technical issue in the kitchen. Within about 30 minutes of my insulin injection and my insulin started to rapidly react to the pre-meal sugars in my body to frightening results – feelings of hunger, severe sweating, shaking, and a mild progression to difficulty thinking. I was experiencing my first moderate Hypoglycemic event.
Fortunately, I was able to consume the recommended dose of DEX4 glucose tablets, and a dose of maple syrup from my running bag, however, not before literally sweating through my clothing and spoiling our dinner out. A moderate to severe hypoglycemia event is truly a #daychanger.
Fortunately, I was able to navigate away from a severe hypoglycemic situation where I was may not able to consume glucose to stabilize my body needing 3rd party assistance such as an emergency Glucagon injection, the recently approved Baqsimi Nasal Glucagon, or even worse emergency medical services.
My bigger concern? What did I do wrong? How could I be better prepared? No one told me about the risks of pre-bolusing. How serious could the situation have escalated if I didn’t have glucose tablets on hand, and more importantly would my girlfriend have known how to have helped if I had not been able to treat myself? Even if I had known about Glucagon, the standard treatment for Severe Hypoglycemia, would she have known how to mix the syringe, or had the confidence to even try?
As Donald Rumsfeld said “there are also unknown unknowns. There are things we don’t know we don’t know.” The simple risks associated with a life relying on insulin was one of them.
Hypoglycemic Education
Recently I was asked by Lilly Canada to represent the T2D community at an education summit on Severe Hypoglycemia held in Toronto. It was an honour to share the room with a handful of some of the most influential diabetics from across Canada, and Lilly spokesperson Crystal Bowersox, a strong T1D and advocate for diabetes education and awareness.

The day with Lilly Canada covered education on hypoglycemia, existing treatment options for moderate and severe hypoglycemia, discussions and panel presentations with some very inspirational T1 Diabetics, information by medical professionals and medical officers from Eli Lilly, and the day ending with an amazing demonstration and discussion with the founders of a recently Health Canada approved treatment of Severe Hypoglycemia called Baqsimi.
Baqsimi: is a new rescue treatment for severe hypoglycemia, demonstrating Lilly’s commitment to simplifying diabetes management through medicines and patient solutions. The formulation was discovered in Canada and is changing the lives of people with diabetes around the world. Baqsimi™ (glucagon nasal powder 3 mg) was approved by Health Canada (Approved January 2020) with ethical status, making it available at the pharmacy with or without a prescription. Baqsimi is indicated for the treatment of severe hypoglycemic reactions when impaired consciousness precludes oral carbohydrates, which may occur in the management of insulin-treated patients with diabetes mellitus, whether Type 1 or Type 2.i Baqsimi is a compact nasal spray that is portable and does not require reconstitution. It is now widely available in pharmacies across Canada.
Lilly Canada, Ready for Rescue – New Nasally Administered Glucagon for Severe Hypoglycemia Available in Canada
What I see as the Benefits of Baqsimi
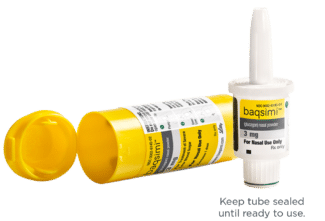
I was amazed by the simplicity of Baqsimi – where traditional Glucagon emergency kit requires the medication to be mixed with a saline solution, then drawn into needle and then injected (See complete instructions here); Baqsimi is a simple nasally administered Glucagon. Anyone, no matter of age, medical experiences, or panic level, should be able to assist their diabetic loved one or stranger through a severe hypoglycemic incident. This is even better for coaches, schools, and all of our diabetes emergency kits.
Learning the Diabetes Ropes from T1D Community
I was honoured to have been able to consult at the Lilly Severe Hypoglycemia Summit, and the topic of hypoglycemia was as engaging as it was informative. More than anything else, and what instantly jumped out at me surrounded by this powerhouse of diabetics; who had travelled from as far as British Columbia and Montreal to attend; is that even as adults living with Type 1 diabetes, individuals who have had decades of experience managing their diabetes (ts all they have known, its a way of life) – yet, even with decades of being insulin-dependent, even diabetic experts make mistakes and need to treat for hypoglycemic events and in some cases have needed medical assistance due to a severe hypoglycemic event.
As a new T1 “like”, T1.5, insulin-dependent T2 diabetic, I have a lot to learn about managing my diabetes, managing my glucose, improving my A1C, and managing both my glucose highs (hyperglycemia) and my glucose lows (hypoglycemia). I hope I will never have to use Baqsimi to treat a severe hypoglycemic event – however, now have the knowledge on how to teach my friends, colleagues, and loved ones, including my 10-year-old, what to do.
As I mentioned a few times over this post – Type 2 diabetes (T2D) education is a challenge and from my perspective still has many holes. However, as a community, we will continue to provide resources and opinions and hopefully give our peers a place to start their own diabetes education journey.
i Diabetes in Canada, Highlights from the Canadian Chronic Disease Surveillance System (11-14-2017). https://www.canada.ca/en/public-health/services/publications/diseases-conditions/diabetes-canada-highlights-chronic-disease-surveillance-system.html
ii Defining and Characterizing the Progression of Type 2 Diabetes. Vivian A. Fonseca, MD (vfonseca@tulane.edu) Diabetes Care 2009 Nov; 32(suppl 2): S151-S156.https://doi.org/10.2337/dc09-S301
iii Diabetes Canada – Severe Hypoglycemia – Last accessed on January 17 – ttps://www.diabetes.ca/health-care-providers/clinical-practice-guidelines/chapter-14#panel-tab_FullText